- © 2018 - 2022 ProVen Probiotics. Cultech
- Contact Us
- Cookie Policy
- Privacy Policy
- Terms and Conditions
What are probiotics?
The human gastrointestinal (GI) tract houses a complex but fairly stable microbial population of more than 1,000 different species of microbes. Each of us has around 100,000 billion viable bacteria living in our intestines, weighing around 1.5kg in total and referred to collectively as the gut microbiome.
The overall relationship of the microbiome to the host is both favorable and beneficial, providing support in the functioning of many parts of our human physiology, including immune and intestinal function.
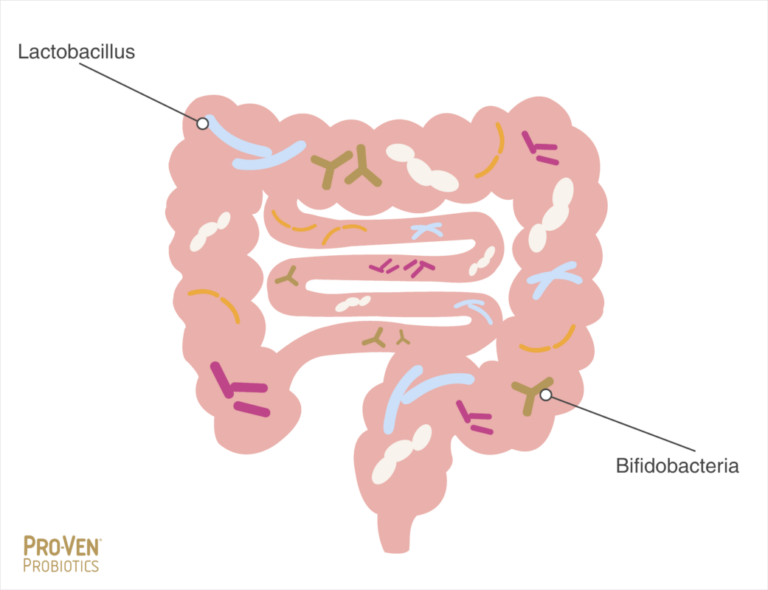
‘Good’ and ‘bad’ bacteria
Within the wide range of bacteria in the gut microbiome, there are species and strains that are beneficial and those that can potentially have a negative impact.
Some types of bacteria in particular, appear to be universally beneficial, providing significant positive effects, as well as having no capacity to become opportunistic pathogens. The two most common species of helpful bacteria found in the human gut microbiome are Lactobacillus and Bifidobacteria.
Under certain circumstances some species and strains can have negative attributes, potentially producing toxins and becoming pathogenic when the opportunity to do so arises (known as ‘opportunistic pathogenicity’).
This pathogenicity can be expressed in situations such as post-operative infections or infection in individuals who are immune compromised. Clostridium difficile (C. difficile) and Escherichia coli (E. coli) are examples of opportunistic strains of bacteria that, under certain circumstances, may become pathogenic and negatively impact health.

Probiotics
Microorganisms, particularly lactic acid bacteria, have been used in food preservation for centuries. The first reports of beneficial effects on human health associated with consumption of Lactobacilli and Bifidobacteria emerged at the beginning of the 20th century.
In the early 1900s, the Russian microbiologist, Elie Metchnikoff, was working at the Pasteur Institute in Paris when he observed that the longest living and healthiest people in the world regularly ate fermented foods, particularly fermented milks. He proposed that fermented foods would support the intestines by providing beneficial bacteria and, as a result, fermented foods gained popularity. Fermented foods containing probiotic bacteria include live yogurt, kefir, sauerkraut and other fermented vegetables.
In 1965, Lilly and Stillwell proposed the term “probiotics” to refer to ‘substances produced by microorganisms which promote the growth of other microorganisms’. Since then, the definition of probiotics has been revised many times and today, the most widely adopted version is ‘live microorganisms which, when administered in adequate amounts, confer health benefits on the host’ (Joint FAO/WHO Expert Consultation, 2001).
The first probiotic supplements were produced in the early 1980s, when interest in the health potential of more concentrated ‘doses’ of probiotic bacteria began. These supplements use probiotic bacteria as proxies for the commensal (normal) bacteria present in our GI tract.
Over the years, many different organisms (bacteria) have been included in probiotics preparations – either singly or in combination. A list of the known common species/strains of bacteria present in our GI tract and used in probiotics products can be seen below.
| Lactobacillus spp. | Bifidobacterium spp. | Other spp. |
|---|---|---|
| L. acidophilus | B. adolescentis | Enterococcus faecium |
| L. brevis | B. animalis subsp. lactis | Enterococcus faecalis |
| L. casei | B. bifidum | Streptococcus thermophilus |
| L. crispatus | B. breve | Bacillus clausii |
| L. delbrueckii subsp. bulgaricus | B. infantis | Bacillus coagulans (L. sporogenes) |
| L. fermentum | B. longum | Escherichia coli Nissle 1917 |
| L. gasseri | Saccharomyces cerevisiae (marketed as S. boulardii) | |
| L. johnsonii | ||
| L. paracasei | ||
| L. plantarum | ||
| L. reuteri | ||
| L. rhamnosus | ||
| L. salivarius |
In addition to research clearly demonstrating the presence of a health benefit, a probiotic for human use needs to demonstrate several characteristics as follows:
• Human origin
• Non-pathogenic
• Non-toxic
• Resistant to stomach acid, bile and pancreatic secretions (enzymes)
• Remain viable during transit through the gastro-intestinal tract
• Attach to human intestinal cells
• Produce an antimicrobial substance
• Achieve the guaranteed shelf life
Probiotic uses
The use of probiotics has been widely investigated and they have been identified as useful for many conditions and functions in the body. Modulation and stabilization of a healthy gut microbiome has been identified as a strategy to prevent both chronic and acute diseases, with research supporting their use for irritable bowel syndrome (IBS), immunity, inflammatory bowel disease, athletic performance, mood and allergy, amongst many other conditions.
As our knowledge of the human microbiome increases, the potential role for probiotics becomes more and more evident across all life stages and many different health conditions.
Genesis 18:8 – Abraham owed his longevity to the consumption of sour milk
76 BC – Roman historian Plinius recommended fermented milk for treating gastroenteritis
1907 – Consumption of the ‘Bulgarian bacillus’ (Lactobacillus bulgaricus) fermented milk was associated with increased longevity and good health
1917 – Escherichia coli Nissle 1917 was used in the treatment of shigellosis and salmonellosis
1930s – ‘Acidophilus milk’ in the USA
1935 – Commercialization of Lactobacillus casei Shirota in fermented milk drink in Japan
1965 – The term “probiotic” (for life) was first used and published by Lilly and Stillwell


 Available from the 8th March to the 19th March on our three most popular women’s probiotics.
Available from the 8th March to the 19th March on our three most popular women’s probiotics.  Discount added automatically at checkout for you.
Discount added automatically at checkout for you. 